Automated Itemized Bill Reviews
CAVO® Itemized Bill Reviews intakes itemized bills and auto-extracts data to increase review productivity by at least 5x. Pairing IB Reviews with Advent Health Partners’ AI-technology enhances the review process even further by supporting your review team with IB-specific machine learning algorithms.
Automated Itemized Bill Reviews
CAVO® Itemized Bill Reviews intakes itemized bills and auto-extracts data to increase review productivity by at least 5x. Pairing IB Reviews with Advent Health Partners’ AI-technology enhances the review process even further by supporting your review team with IB-specific machine learning algorithms.
CAVO IB Reviews turns the manual, laborious process of reviewing itemized bills into one that can be completed quickly and efficiently. CAVO uses OCR to read thousands of IB formats and standardize their data, enabling review teams to sort and filter, make line adjustments, create auto-generated provider reports, and more, all on one screen. Streamlining the IB review process with CAVO results in review productivity lifts of five to fifty times greater than the process without, saving both time and money.

Decrease Costs
- Cost savings on incremental reviews
- Reallocate data entry resources to higher value activities
Increase Reviews
- Increase productivity of provider bill review team
- Dramatic decline in time per review enables increase of pre-pay reviews

Create Efficiencies
- Negate the need for itemized bill transcription
- Replace manual page-by-page review with online hospital bill search
What is CAVO IB Predict?
CAVO IB Predict uses Natural Language Processing (NLP) technology to review and recommend prioritization of denied line item charges before the reviewer even looks at a claim. Reviewers can view the detailed reasons for flagged line item charges, and within the same view, easily accept or reject each recommendation. CAVO IB Predict utilizes these decisions to continuously enhance the machine learning model with customized rules that you can manage directly within the application.
The engine is prebuilt with industry edits including MUE, PTP, routine non-covered supplies, POC services, and non-payable benefits. Using CAVO IB Predict with CAVO technology takes your itemized bill review process to the next level with even greater efficiencies and higher productivity.
Benefits of CAVO IB Predict
Positively Impact Financials
- Catalyst to pre-pay reviews
- Expand savings

Increase Staff Productivity
- Move to validation instead of determination
- Increase consistency in review processes and outputs
Continually Refine ML Model
- Move toward automation
What Makes Advent Health Partners Different?
Advent delivers a one-vendor solution that brings together data science expertise, review-specific technology, and most notably, claims review expertise to assist you with your itemized bill review process. Utilizing API hooks, the CAVO IB Predict model incorporates AHA, AMA, and CMS guidelines in addition to Health Plan specific guidelines.
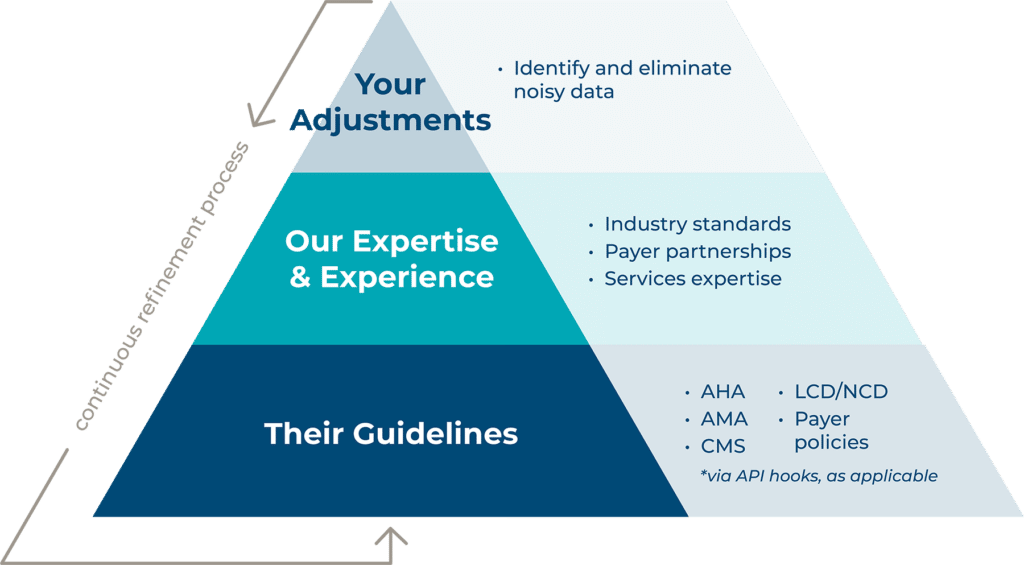
Advent’s expertise and experience in the space lead to an initial model tailored to specific trends in the data from the start, a model that is then continually refined to eliminate noise and deliver the most optimal results for your plan as possible
Visit our Knowledge Center for the latest articles, videos, news and upcoming events.
Get in touch to discover how Advent Health Partners can help your organization tackle its business challenges.
Please submit the form below, and one of our experts will be in touch shortly.
